Call to speak to a Licensed Insurance Agent
Mon - Fri 8am – 8pm EST; Sat - Sun 10am - 6pm EST
Call to speak to a Licensed Insurance Agent
Mon - Fri 8am – 8pm EST; Sat - Sun 10am - 6pm EST
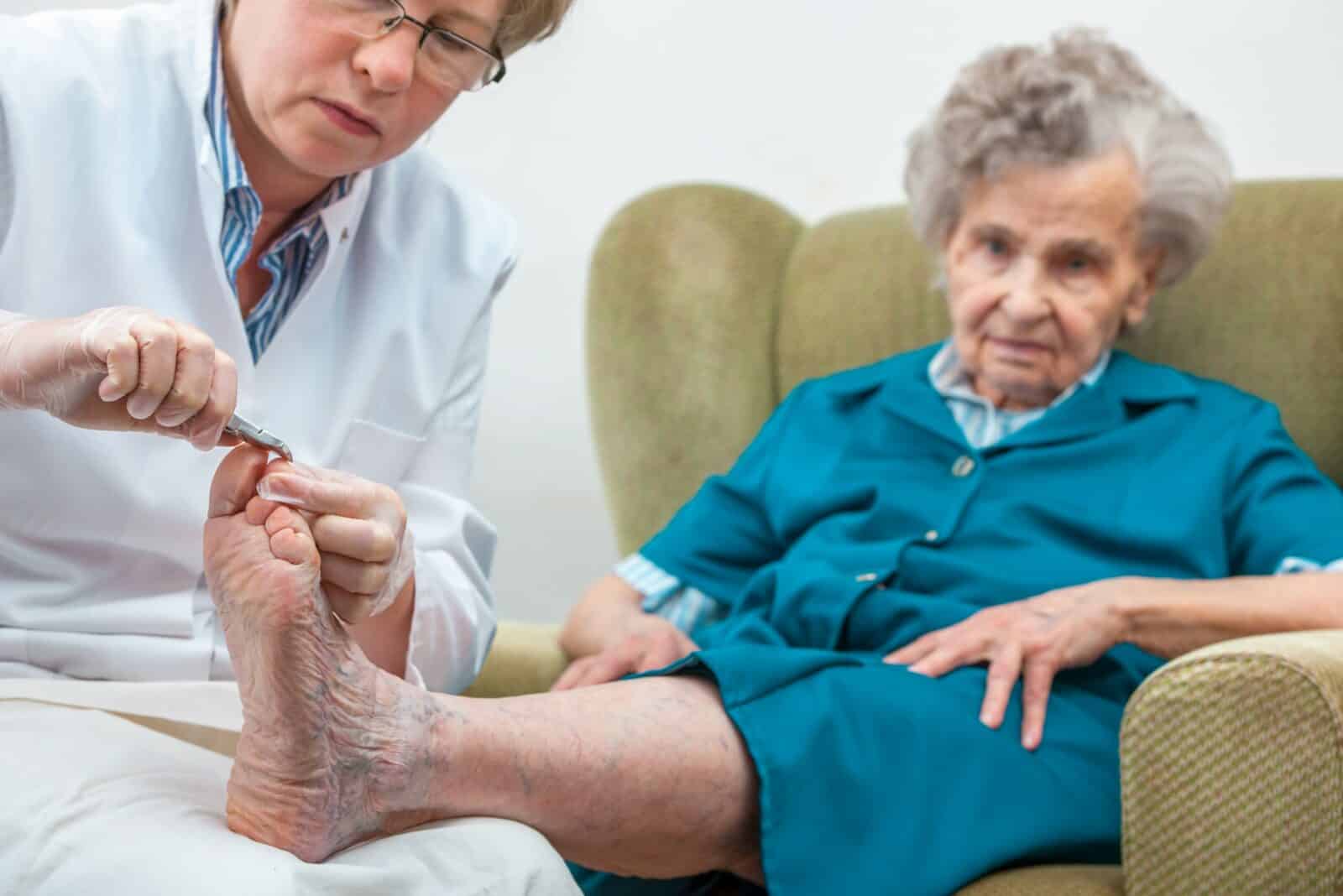
When there is an injury or other medical condition in our foot, obviously we have to get it taken care of. And, most of the time, Medicare will, ummm, foot the bill. But some foot care services are not really for treating ailments. So what happens when it comes to routine foot care?
This leads to a question that many have which is, “Does Medicare cover routine foot care?” Below you’ll get the answer to that and much more.
The short answer is no. In most cases, Medicare will not cover the cost of routine foot care. That said, there may be some situations where you can get these costs covered. Below we’ll take a closer look at this to see when you might be able to get Medicare to pay for your routine foot care.
Original Medicare (Medicare Part A and Part B) does not provide coverage for routine foot care. Original Medicare does not provide coverage for routine foot care because most of the time they do not provide coverage for services that are not medically necessary.
Original Medicare does not provide coverage for routine foot care services such as nail trimming, treatment of calluses, or pedicures.
However, Original Medicare may provide coverage for some foot care and services if it is medically necessary. It must first be ordered by your healthcare provider to be eligible for coverage, however. Some foot conditions that may be covered include treating wounds, infected nails, or hammertoe.
Original Medicare also provides coverage for routine foot care if you have diabetes. They provide coverage for treatment for diabetic neuropathy.
Coverage for foot injuries or diseases is provided by Part A if it takes place in an inpatient setting. Medicare Part A will cover 100 percent of the costs of hospital stays for up to 60 days. For days 61 to 90, Medicare Part A will still provide coverage. However, you will pay a copayment of almost $400 per day. After 90 days, Medicare Part A will no longer provide coverage.
However, Medicare Part A provides 60 lifetime reserve days. If you have them, they will still provide coverage for your hospital stay after 90 days, but you will pay for a copayment of close to $800.
On the other hand, coverage for routine foot care is provided by Medicare Part B if it takes place in an outpatient setting. Medicare Part B covers 80 percent of the costs of covered routine foot care. You will pay for the remaining 20 percent as coinsurance or copayment.
While you may not get coverage for routine foot care through Original Medicare, there are many Medicare Advantage plans (Medicare Part C) that will provide coverage for it. At a minimum, these plans must cover all the same things that Original Medicare covers.
However, these plans also offer coverage for things that Original Medicare does not. And routine foot care / podiatry services is often one of those things. That said, you’ll need to check with your Advantage plan as coverage and costs will vary from plan to plan.
Note: Medicare coverage changes all the time. And your specific coverage may vary from plan to plan for Medicare Advantage and Medigap plans. Always be sure to double check with your health care provider and/or Medicare insurance provider about what your plan covers and what it does not.
This article is part of our series on “What does Medicare cover?”
Also, you can check out other articles in this series including: Does Medicare cover InterDry?