Call to speak to a Licensed Insurance Agent
Mon - Fri 8am – 8pm EST; Sat - Sun 10am - 6pm EST
Call to speak to a Licensed Insurance Agent
Mon - Fri 8am – 8pm EST; Sat - Sun 10am - 6pm EST
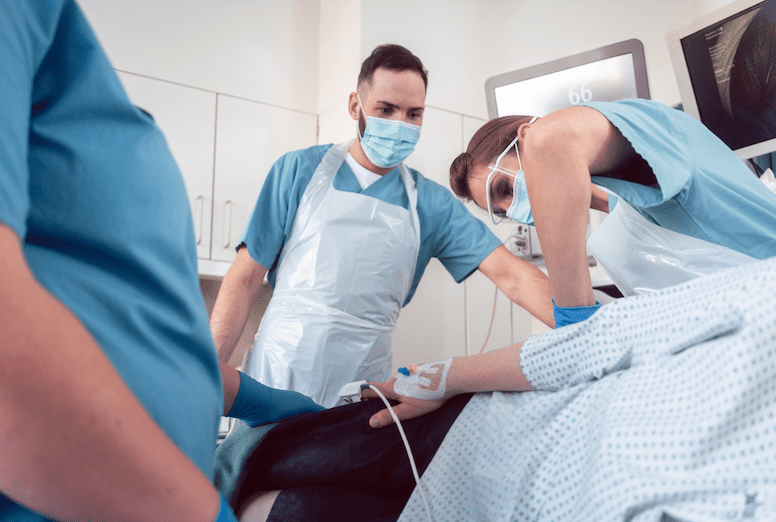
A colonoscopy is an important health screening procedure that can help prevent, identify, and treat colon cancer by removing polyps or precancerous growths.
Physicians use a colonoscopy to detect disease, alterations, or anomalies in the colon and rectum.
It is recommended everyone over the age of 45 get a colonoscopy so a common question many people have is, “Does Medicare cover a diagnostic colonoscopy?”
In this article, we answer the question in clear, plain English. You will also find the average costs of a diagnostic colonoscopy and other helpful info.
The short answer is yes; Medicare does cover the cost of a diagnostic colonoscopy. That being said, they do not do so 100% of the time.
As is often the case with Medicare, certain conditions have to be met for Medicare to pay for your diagnostic colonoscopy. Below we look at what these are so you know what to expect.
First, it’s important to understand the difference between a preventative colonoscopy and a diagnostic colonoscopy.
Preventative or “screening” colonoscopies are done to in order to try to prevent colon cancer. They are a preventative health service and considered an essential health benefit under the ACA.
A diagnostic colonoscopy is one that is performed only after abnormal symptoms or test results. It is done in order to investigate these abnormalities to determine if cancer is present.
Original Medicare (Medicare Part A and Part B) provides coverage for a diagnostic colonoscopy.
This plan provides coverage for your diagnostic colonoscopy if it is medically necessary. Your healthcare provider must first order the test for Original Medicare to provide coverage.
It is important to know that coverage for a preventive and diagnostic colonoscopy is different.
For preventive colonoscopies, most of the time, Original Medicare covers 100 percent of the costs of preventive colonoscopies. But, they only provide coverage for the screening every 24 months if you are considered at high risk of colorectal cancer.
They provide coverage for a flexible sigmoidoscopy every 48 months, and a colonoscopy every 120 months if you are not considered at high risk of developing colorectal cancer.
So, when is it covered by Part A vs. Part B?
Diagnostic colonoscopies are covered by Medicare Part A if they take place in an inpatient setting such as a hospital or a skilled nursing facility.
If the diagnostic colonoscopy is covered under Medicare Part A, you may pay a deductible or a copay.
Most of the time, coverage for diagnostic colonoscopy is provided by Medicare Part B.
For diagnostic colonoscopy, Medicare Part B covers 80 percent of the costs of your diagnostic colonoscopy.
So, how do you determine if it is a preventive or diagnostic colonoscopy? Well, most colonoscopies are considered preventive.
Sigmoidoscopy and screenings are considered preventive screenings. However, if polyps are found and removed, it becomes a diagnostic colonoscopy.
Finally, Medicare Advantage plans (Medicare Part C) provide coverage for diagnostic colonoscopies. They must cover everything Original Medicare does.
However, they will also cover services, treatment, tests, etc that Original Medicare does not. Exactly what a plan will cover and how much the out-of-pocket costs are will vary from plan to plan.
The national range of a colonoscopy costs generally cost between $1,250 to $4,800. The national average cost of this screening is $2,750.
During a colonoscopy, a physician examines the large intestines by inserting a thin, flexible scope into the rectum. Then they push it through the colon. The scope is equipped with an illuminated camera that captures the large bowel lining images. Finally, it identifies any abnormal growths or polyps.
Note: Medicare coverage changes all the time. And your specific coverage may vary from plan to plan for Medicare Advantage. Always be sure to double-check with your health care provider and/or Medicare insurance provider about what your plan covers and what it does not.
This article is part of our series on “What does Medicare cover?”
Also, you can check out other articles in this series, including: Does Medicare cover Rhopressa?