Call to speak to a Licensed Insurance Agent
Mon - Fri 8am – 8pm EST; Sat - Sun 10am - 6pm EST
Call to speak to a Licensed Insurance Agent
Mon - Fri 8am – 8pm EST; Sat - Sun 10am - 6pm EST
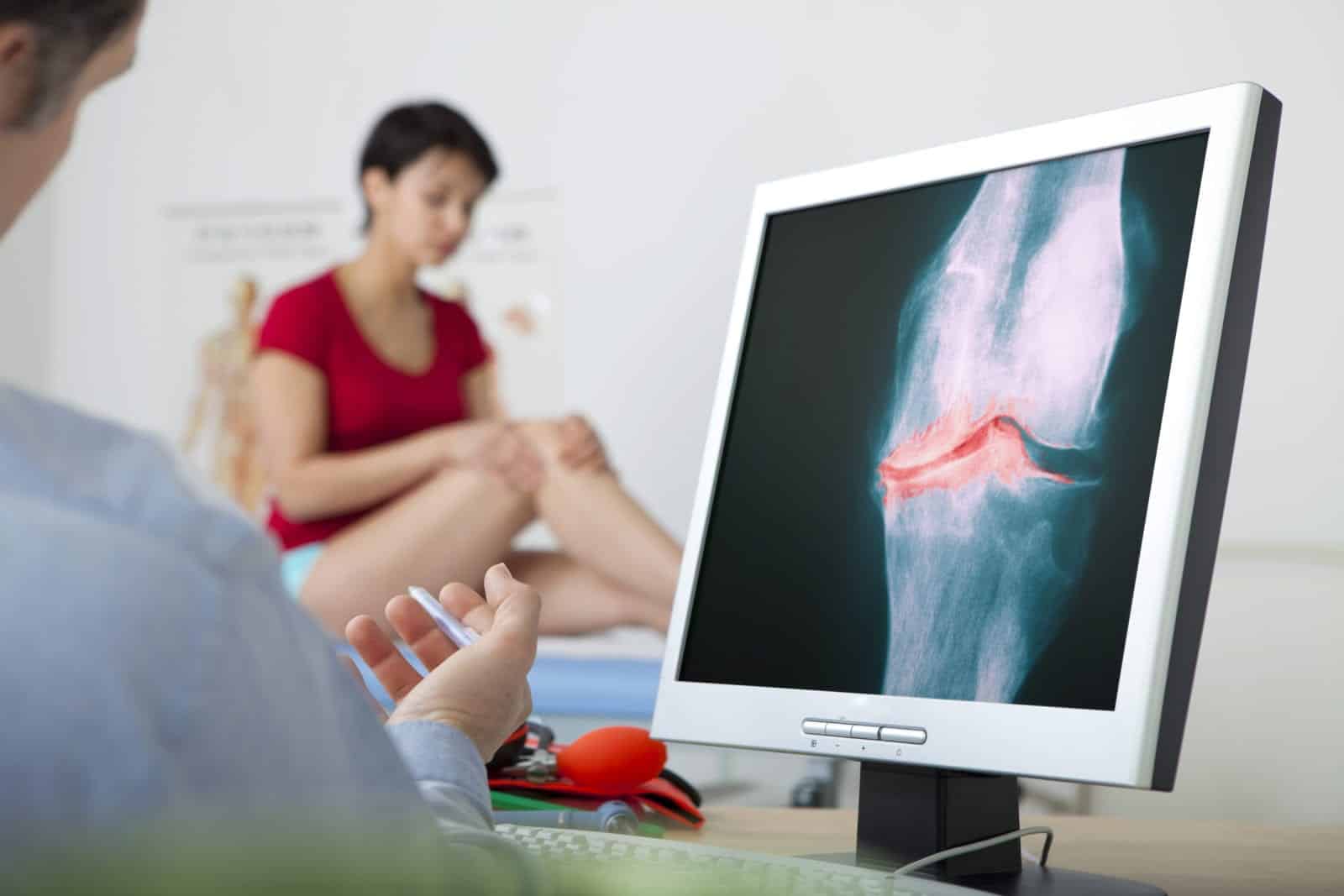
Curious about Coolief Knee Treatment and Medicare coverage? Yes, Medicare can help pay for it, but not always. Like following rules, certain conditions must be met for Medicare to help with costs. This article explains these conditions, giving you a clear idea of what to expect.

If you’re thinking about Coolief Knee Treatment and if Medicare covers it, you’re in the right spot. We know that medical costs can be overwhelming, and it’s important to know if Medicare covers this treatment. We’ll dig into the info you need, so you can make smart choices for your health.
If you want to know if Coolief Knee Treatment is covered by Medicare, this article has the answers. It explains important info to help you make crucial decisions about your healthcare.
Some of the things you’ll learn about Coolief and how it works with Medicare are:
Embark on an educational journey towards informed healthcare choices. Dive into the article to equip yourself with essential insights.
The short answer is yes; Medicare may cover the cost of Coolief knee treatment. But not 100% of the time. As is often the case with Medicare, certain conditions have to be met in order for Medicare to pay for your Coolief knee treatment. Below we look at what these are so you know what to expect.

Even though Medicare may cover Coolief knee treatment, we recommend that you confirm this first with your healthcare provider as well as your insurance provider.
In the treatment’s clinical study, it is shown that it is long-lasting and it provides more significant pain relief compared to steroids. But because it’s a newer treatment you’ll want to discuss your options first with your doctor.
Both to find out if Medicare will cover the procedure and also so you’re aware of risks of the treatment.
Coolief is a procedure that treats chronic knee pain through a minimally invasive approach. This involves injecting a cold solution into the knee joint to numb pain nerves.
However, not everyone with chronic knee pain is considered a candidate for Coolief, as it’s not deemed medically necessary for all cases. Medicare Part B specifically covers procedures and surgeries that are medically necessary. This means the procedure must fulfill these conditions:
1. Diagnose or Treat a Medical Condition: The procedure should be essential for diagnosing or treating a medical issue.
2. Likely Effective: The procedure is expected to have a positive effect on the medical condition.
3. Not Experimental: The procedure is established. This means it is not in the experimental or investigational stage.
4. Benefits Outweigh Risks: The benefits of the procedure should outweigh any potential risks or side effects.
Coolief might not be covered by Medicare Part B because there are other treatments for chronic knee pain that have been around longer and are considered to work better. For example, getting a knee replacement is usually seen as a better option for really bad knee pain.
Medicare has to be careful with its money and usually only pays for treatments that are proven to work well and are good value for the price. Since Coolief is still pretty new and we don’t yet know how well it works in the long run, Medicare might not see it as a good use of its funds.
If you’re thinking about trying Coolief, talk to your doctor first. They can help you understand if it’s a good option for you by discussing the good and bad sides of the treatment. They can also let you know if your insurance will help pay for it.
For questions about Coolief’s coverage Medicare, feel free to reach out to your doctor or your Medicare insurance plan for more information.
If you’re a Medicare Part B beneficiary considering Coolief, here are some steps to consider:
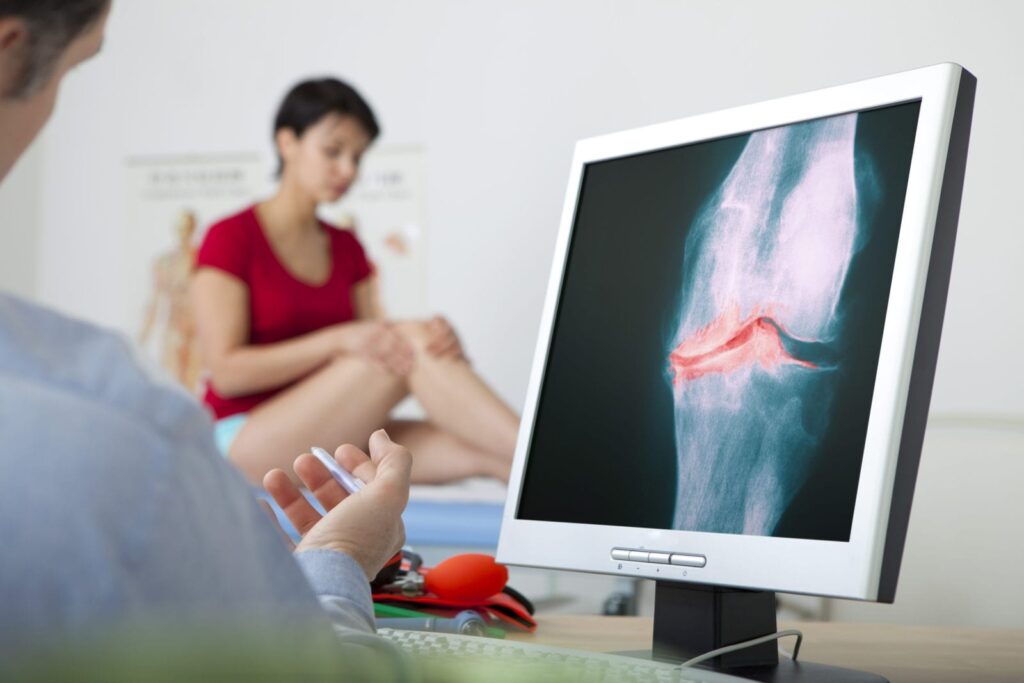
Consult your doctor about pain relief options covered by your Medicare plan. These include options such as physical therapy, injections, and medications.
Ask if your plan allows exceptions for procedures like Coolief that might not be standard.
Coolief’s cost typically ranges from $2,000 to $5,000. If you can afford this, you might consider covering the expense yourself.
Organizations offer financial help to those needing Coolief but facing affordability issues.
Coolief Website: Learn more about Coolief on their official website
Medicare Website: Get more insights from the official Medicare site
Patient Assistance Program Finder: Discover potential financial assistance
Coolief knee treatment cost typically is somewhere between $2,000 to $4,000 according to NBC News.
If you’re looking to manage the expenses of the Coolief procedure while paying out-of-pocket, here’s how to go about it:
1. Get Quotes: Reach out to the providers – the physician, facility, and anesthesia – to know their respective charges.
2. Negotiate Pricing: Since you’re paying directly, you might be able to discuss and potentially lower the costs in certain cases.
3. Consider Surgery Centers: Opting for a surgery center over a hospital could lead to reduced facility expenses.
4. Talk With Billing: The billing team is likely well-equipped to guide you on cost-saving measures.
Remember, not all insurance plans cover the Coolief procedure. If you’re paying out-of-pocket, there might be financial aid available through your health insurance provider or other organizations.
When it comes to covering the cost of Coolief treatment, there are various approaches you can consider. Here are some practical tips to help you navigate the financial aspect of your journey:
1. Health Savings Account (HSA): If you have a health plan with a high deductible, a Health Savings Account (HSA) might be a good idea for you. The money you put into an HSA isn’t taxed, and you can use it to pay for approved medical costs. This includes a treatment called Coolief.
2. Payment Plans: Some doctors and hospitals let you pay for treatments little by little, each month, instead of paying everything at once. This helps you spread out the cost over a set amount of time.
3. Healthcare Credit Cards: Healthcare credit cards help you pay for medical expenses. They sometimes let you go a while without paying interest, making it easier to afford Coolief treatment.
4. Commercial Insurance: If you have regular insurance, you should call them to see if they’ll help pay for Coolief treatment. Sometimes, you may need to get permission from your insurance company before you get the treatment.
Coolief treatment, or cooled radiofrequency ablation, is a minimally invasive treatment. It works by transmitting pain signals placed near the knees’ nerves. Your doctor will insert electrodes through the skin that deliver heat to the nerve.
The procedure hinders the nerves’ ability to send pain signals to the brain. Aside from heating up the electrodes, Coolief treatment also cools them down.
Even though the procedure is minimally invasive, it requires multiple injections and x-ray guidance. This is to know where precisely the electrodes should be injected.
Coolief’s clinical studies show that the treatment can provide pain relief for long-lasting periods, up to 1 year. Patients have also reported feeling pain relief 1-2 weeks after the procedure. More than that, these studies show that it improves the lives of people suffering from osteoarthritis.
Coolief treatment does not require an overnight hospital stay. As soon as the procedure is over, patients can immediately return home. Unlike surgery, this type of treatment does not require an incision.
Most Coolief treatment studies have shown that it rarely shows side effects. However, the manufacturer still warns of potential risks. These may include infection and nerve damage. But the potential risks may be based on reports of the procedure being performed on other parts or areas of the body.
It is also important to know that Coolief treatment is the first and only radiofrequency treatment for osteoarthritis that the FDA clears. But despite that, it is important to discuss it with your doctor before undergoing Coolief treatment.
Exploring Medicare-Covered Alternatives to Coolief
Medicare offers coverage for various pain management and interventional treatments beyond Coolief. Here’s a breakdown of these options:
These injections are a common approach to alleviating knee pain by reducing inflammation. Medicare may cover them if they’re medically necessary.
Providing temporary relief, these injections numb the nerves around the knee. Medicare’s coverage depends on medical necessity.
This minimally invasive surgery lets doctors examine the knee’s interior, allowing tissue removal or cartilage repair. Medicare may cover it if deemed medically necessary.
This surgery replaces worn knee parts with artificial components, offering long-term pain relief. Medicare’s coverage depends on medical necessity.
Each treatment varies in efficacy, cost, and benefits. Steroid injections are budget-friendly but might offer less relief. Genicular nerve blocks provide better relief, though they might require more frequent repetition.
Arthroscopy offers lasting relief, but at a higher cost. Total knee replacement is the priciest but most enduring solution.
The optimal treatment depends on factors like your health history, pain severity, lifestyle, and expectations. Consult your doctor for personalized guidance, considering your specific Medicare plan’s coverage.
The first step to ensuring that Medicare will pay for Coolief knee treatment is to discuss it with your healthcare provider. They can help you determine if the treatment is right for you and if it is likely to be covered by your plan. They can also help you with the preauthorization process, which is required for some Medicare plans.
To check if your Medicare plan covers Coolief, you can contact your plan directly or you can use the Medicare Coverage Database. The Coverage Database is a searchable database of all Medicare-covered services and procedures. You can search by the name of the service or procedure, or you can browse by category.
If your Medicare plan initially denies coverage for Coolief, you have the right to appeal the decision. You can appeal the decision yourself or you can have your healthcare provider appeal on your behalf. The appeal process can be complex, so it is important to get help from your healthcare provider or from a Medicare advocate.
Here are some additional tips for navigating Medicare coverage for Coolief knee treatment:
So, this article went in depth about if Medicare will cover Coolief Knee Treatment or not. We looked at what Medicare covers, other ways to treat pain, if Coolief is the right fit for you, and how to deal with payment stuff.
Now you know more and can make better choices about your healthcare. Going ahead, you might want to talk about what you’ve learned, get advice from a doctor, or read more articles like this one. You’re just starting to figure out your healthcare options, so go ahead and take the next step. You got this!
No, Coolief uses water cooling while heating nerves. Coolief is unlike other methods of radiofrequency ablation. Coolief’s water circulation helps create a larger lesion. This results in easing nerve ablation without overheating body tissue.
After Coolief treatment, 2 out of 3 patients saw a 50% drop in knee pain and 83% fewer arthritis symptoms. Plus, people felt better in daily life. FDA approved COOLIEF for chronic knee pain from osteoarthritis.
COOLIEF* has shown to greatly boost physical function and life quality in knee patients with OA for up to 12 months. Any discomfort is usually eased with over-the-counter pain meds. Most get back to daily life in a few days and feel pain relief within 1–2 weeks.
COOLIEF is a surgery-free option, meaning no cuts or general anesthesia. It’s a quick procedure, around an hour, but you’ll need someone to drive for you afterward. Expect slight pain and swelling later. The process involves using radio waves to stop pain signals by deactivating certain nerves.
Possible risks of radiofrequency ablation:
Rare nerve and blood vessel damage causing bleeding or numbness.
Heat damage to nearby structures.
Rare permanent nerve damage or worsened pain.
Uncommon infection or bleeding at needle site.
If your doctor says you need it, Medicare might pay for radiofrequency ablation. If it’s done as an outpatient, Medicare Part B usually covers it. You’ll usually pay 20% of the cost plus deductible and monthly premium.
Also, you can check out other articles in this series including Medicare coverage for Zilretta, hypnotherapy and more.